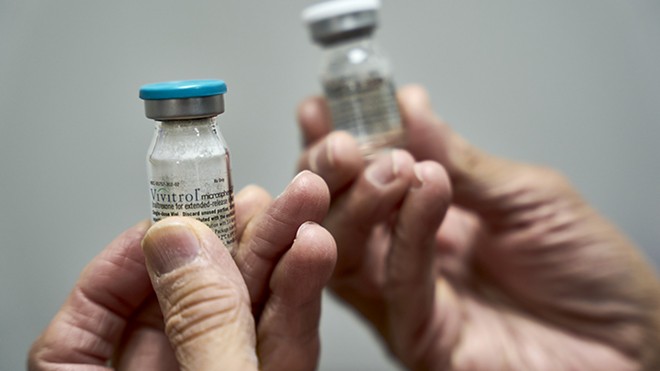
A controversial opioid treatment drug comes to the fore
Daniel Coverdell knows well the neighborhood surrounding Jubilee Community Church off of North Grand Avenue.
In the bad old days, only a few months ago, Coverdell would drive his Dodge Ram pickup truck through nearby northside streets looking for black-market fentanyl, the synthetic painkiller 100 times more powerful than heroin.
“This is where I came to score all my dope,” says Coverdell, 42, of Rolla.
Coverdell knew he risked an overdose death each time he consumed fentanyl. Determined to stay alive for his young sons, he decided to get clean.
After an intensive detox program, he began attending daily support meetings and surrounded himself with other sober people at the newly opened treatment center and clinics at Jubilee Community Church.
He also began taking monthly injections of Vivitrol, the brand-name version of the opioid-blocker drug naltrexone.
Clean cut and polite, Coverdell is a Marine veteran who looks you straight in the eye and answers your questions with a sharp “Yes, sir,” and “No, sir.”
Yet for more than twenty years Coverdell has battled his dependence on opioids. It began shortly after he left the Marine Corps and was living on the East Coast. His addiction began innocuously enough: After a night of drinking, a friend offered him a Vicodin pill, a prescription painkiller, as a way to recover from a hangover.
“It helped,” he recalls. “It made me feel better.”
After moving back to his hometown of Rolla, he progressed to OxyContin, another prescription painkiller, but more powerful and addictive. Soon, it consumed his life.
“It just really made you feel numb,” he says. “It made me feel good. It gave me some energy. In my mind, it told me I was sharper and funnier and more enjoyable to be around.”
Four years ago, Coverdell moved on to fentanyl after a government crackdown drove up the price of black-market OxyContin.
Today, even though he knows he could walk out the door to Jubilee and within a few minutes find someone who’d sell him heroin or fentanyl, Coverdell says he has no interest in doing so.
“If I didn’t have Vivitrol, I’d just sit there and think about it, and your thoughts would almost consume you,” he says. “And now I don’t think about it.”
For the first time in a long time, Coverdell says he looks to the future with hope.
“For me, personally, I think Vivitrol is the way to go.”
A bill introduced in the Missouri Senate a few weeks ago could go a long way toward making naltrexone available for a vastly wider target population. The measure would allow the state to create a standing order to allow anyone to buy naltrexone without a prescription at any pharmacy in the state.
As a result, people most at risk for developing either opioid use disorder or dying from a fatal overdose — people with a family history of substance use, say, or whose tolerance for opioids has diminished after leaving prison or a treatment program — could use naltrexone prophylactically, in the form of daily pills that cost less than $1 apiece.
If the measure is signed into law, Missouri would be the first state to allow consumers to buy naltrexone over the counter and use it preventively on a long-term basis to prevent opioid overdoses, either for themselves or others.
In effect, the law would make Missouri a laboratory for a new strategy to fight America’s raging opioid epidemic. But there are risks.
Percy Menzies, the president and cofounder of Assisted Recovery Centers of America of St. Louis, which runs Jubilee’s medical-based treatment center, said that using naltrexone as part of a campaign of prevention is well worth the effort.
After all, America’s opioid crisis is spiraling out of control with no end in sight. For the 12-month period ending in April 2021, more than 100,000 Americans died from drug overdose deaths — a record number, and a five-fold percent increase in overdose deaths since 2000. (Experts say the actual number of recent deaths may be much higher.)
Most of the surge in OD deaths is being powered by the widespread introduction of fentanyl into America’s black-market drug supply.
Fentanyl is being covertly mixed with cocaine, methamphetamine and even counterfeit versions of Percocet and Xanax. Which means that many of the people dying from drug overdoses don’t even know they’re ingesting fentanyl.
“Fentanyl is so dangerous,” Menzies says. “And it is now lacing [almost] every drug. It is almost like a variant of a deadly virus that is killing people left, right and center.”
Opioid abuse was once considered a predominately white scourge. At about the same time that crack cocaine was decimating Black neighborhoods, in the mid-1990s, the drugmaker Purdue Pharma launched a new opioid painkiller called OxyContin and began aggressively marketing it to rural areas filled with people suffering from debilitating injuries, such as coal miners.
Not coincidentally, West Virginia became ground zero for the drugmaker’s marketing push, which depended on a web of complicit drug distributors, pharmacies, sales reps and government regulators.
OxyContin almost immediately was hailed as a medical breakthrough. That’s because Purdue Pharma promised the Holy Grail of pain relief: a single pill with a proprietary release mechanism that could provide powerful day-long relief to those suffering the most agonizing forms of injury or disease, such as bone cancer, yet safe enough to prevent addiction.
Purdue Pharma’s promises, however, amounted to a mountain of lies, as shown by wave after wave of civil lawsuits, multi-billion-dollar legal settlements and criminal prosecutions over the past two decades.
But they were incredibly lucrative lies that enabled the Sackler family, Purdue’s owners, to reap billions of dollars in profits from OxyContin sales that showered millions of pills on rural America.
In recent years, with the help of fentanyl and the isolation caused by the COVID-19 pandemic, opioid use has surged in urban areas and has hit America’s Black population especially hard, touching off waves of overdose deaths nationwide.
Overdose deaths among Black men and women increased in 2020 at three times the rate of white people, soaring more than 33 percent. Especially hard hit are Black men in Missouri; they are four times more likely than a white person to die of a drug overdose.
In the city of St. Louis alone, almost 900 people have died from deadly drug overdoses over the past two years.
If passed into law, the bill pending in the Missouri Senate would allow naltrexone to be distributed in much the same way as naloxone (brand name: Narcan), a drug that is used to reverse opioid overdoses. People can go to a pharmacy and buy Narcan with no questions asked, either to use personally or on others at risk of an opioid overdose.
The bill is sponsored by state Senator Holly Rehder, R-Sikeston, who has been outspoken for years about the struggles her own family members, including her daughter, have gone through with substance use disorders.
“It would be much like we did with naloxone,” Rehder says of her proposal. “It’s really modeled after that.”
Rehder’s bill is targeted at people in substance recovery who, because of a sudden life stress, such as a parent’s death, are at acute risk for relapse.
So her bill “would give them the ability to go get this medication, take it and really just stave off that possibility of failing,” Rehder says.
Naltrexone is also used to combat alcoholism. It has shown great success by allowing problem drinkers to take a pill that helps them avoid going too far with their drinking.
The federal government approved naltrexone’s use as a medication to treat opioid addiction in 1984. But since then it has been overshadowed by the other two medications traditionally used to treat opioid use disorder: methadone and buprenorphine, whose brand name is Suboxone.
Both drugs are staples of opioid treatment clinics nationwide. Methadone and buprenorphine are addictive opioids in themselves — but considered safer than street heroin or fentanyl.
Vivitrol, in contrast, is not addictive. But it is controversial among addiction experts because, for one thing, users can’t start taking it until all opioids are gone from their system, which can take a week or longer.
For this reason, Alkermes, the Waltham, Massachusetts-based maker of Vivitrol, has focused much of its promotional efforts on the nation’s drug courts and jail and prison systems. Prisoners, upon their release, usually have no opioids in their systems, and thus are prime candidates for Vivitrol.
Menzies, however, wants to raise the profile of naltrexone and make it much more widely available. He sees Rehder’s bill, which is the result of discussions he’s had with the senator, as an important start.
One of the things that bothers Menzies about current solutions being offered for opioid abuse is the fact that naltrexone is offered to well-to-do patients, while methadone and buprenorphine are offered to low-income people in treatment programs.
“If you’re a physician, you cannot go back to practicing medicine if you’re on methadone,” Menzies says. “But you can go on naltrexone. If it’s good for the physician, why isn’t it good for the prisoner?”
Last March, the pop singer Demi Lovato revealed she had been receiving monthly injections of Vivitrol after suffering a near-fatal overdose in 2018 caused by drugs laced with fentanyl.
Lovato said in an interview for a recent documentary that the medication is something that can help her on the difficult path of addiction recovery.
“At least for a few years, it can’t hurt me,” Lovato says in a documentary.
The fact that methadone and buprenorphine can cause lifelong dependency is a reason many drug clinics promote the use of those medications, according to Menzies.
“There are special interest groups that want to continue to promote addiction as an incurable disease,” he says. “There’s a very strong financial motive to keep somebody in the same state. So treatment is done on a financial model, on a business model, but not on an outcomes-based model.”
Menzies adds, “Giving somebody an addicting drug is a lot more profitable than giving somebody a non-addictive drug. That’s the bottom line.”
Naltrexone can make a huge difference, saving lives at a time when many are dying needlessly, he says.
“That is why it makes me so angry,” Menzies says. “When we are fighting a war, every weapon has to be utilized. And we have to use the weapons creatively.”
Naltrexone works by blocking the brain’s opioid receptors, preventing the symptoms of opioids from taking effect. It is taken either in pill form or as an intramuscular injection, usually in the buttocks.
It has earned the nickname “the steel spike” for good reason.
“Because once you give them the naltrexone, it binds so strongly with the opiate receptors, that nothing can displace it,” Menzies says.
A pharmacist by training, Menzies has a long history with naltrexone. He worked in the marketing arm of the pharmaceutical subsidiary of chemical giant Dupont that previously marketed the drug.
One of naltrexone’s biggest assets is the fact it has no street value and no potential for abuse. That’s in stark comparison to methadone and buprenorphine, which users sometimes trade for heroin or synthetic painkillers.
Nonetheless, naltrexone has some major drawbacks. Patients must be completely detoxed from opioids, and many are reluctant to take naltrexone because it doesn’t give them the slight high they experience with methadone and buprenorphine.
“Because the thing with addiction is that anything that affects your survival instinct, the biological instinct for survival, is very difficult to treat,” Menzies says. “Because the addiction has gone and said, ‘You need the drug to survive. If you don’t take it, you’re going to die.'”
In recent years, however, evidence of another major drawback about naltrexone has emerged. Patients who quit naltrexone are at increased risk of overdose and death because their tolerance for opioids has dramatically diminished, according to a 2018 article published in the journal Drug Safety.
Because Vivitrol is so effective at deterring people from abusing opioids while on it, over time it drastically reduces their tolerance for them — unlike methadone and buprenorphine. This means that those who relapse after a period on Vivitrol are at a particularly high risk of overdosing, the journal reported.
Dr. Evan Schwarz, an associate professor of emergency medicine at Washington University School of Medicine, voiced concerns about how a prolonged period of opioid abstinence on naltrexone could make a recovering opioid user vulnerable to a fatal overdose, especially if fentanyl is involved.
“That’s part of the problem with naltrexone,” Schwarz says. “If you’re not careful, you drop someone’s tolerance, and you go out and purchase fentanyl or one of those fentanyl derivatives, you’re at a huge risk of overdosing because they’re so potent.”
He emphasized he has nothing against naltrexone. Nor is his warning a criticism of Rehder, whom he praised for her legislative accomplishments, including sponsorship of bills to make naloxone available over the counter, to make needle exchanges legal and to set up a statewide prescription drug monitoring program.
But Rehder’s bill, Schwarz says, “may need a little bit more discussion to figure out how we’re actually going to use this to try to prevent from hurting the people we’re trying to help.”
For his part, Menzies acknowledges that people on Vivitrol face a risk from overdose if they relapse and abruptly stop taking the medication.
But serious medical problems can occur for anyone who stops taking a crucial medication, such as people at risk of stroke who stop taking blood thinners or diabetics who stop taking insulin.
“That can happen with anything,” Menzies says. “That doesn’t mean you don’t use it at all.”
It’s the same situation for opioid users who lose their tolerance after an extended stay in jail.
“So does that mean you never release them from jail?” Menzies says.
The state-funded ARCA clinic at Jubilee Community Church opened in October in the husk of an abandoned grocery store adjacent to the church.
The clinic launched after a trial run with a mobile clinic parked outside the church.
Assisted Recovery Centers of America’s treatment program, which can last up to eight months, includes medication, therapy, job skills training and counseling. Housing is provided at the nearby Turner House, where Coverdell works as a manager, or Victory Over Bondage group home, which is a few blocks down the street.
Smartpac, a St. Louis County-based packaging company, has hired 35 patients from the ARCA/Jubilee partnership.
The collaboration between ARCA and Jubilee began when the church’s senior pastor, Bryan Moore, met with Menzies.
“He said he had an idea, and I kind of agreed,” Moore says. “And we kind of matched kindred spirits and said, ‘Let’s get it done.’ It’s as simple as that.”
The treatment center’s impact was clear from the start, Moore says.
He describes his entire ministry as a “reentry program” in which “you can come off the street, addicted. And we put you back to purpose and destiny. That’s what the entire ministry is designed for.”
“What is amazing,” Menzies says, “is that when you talk about treatment, the first thing you hear is, ‘Not in my backyard. We don’t want you here.’ There is such hostility towards that. This man said, ‘I want you in my front yard.'”
Fred Rottnek, ARCA’s medical director and an addiction expert, helped Rehder draft the bill opening up access to naltrexone.
The prophylactic use of naltrexone would be similar to the use of Prep for people with HIV, according to Rottnek, a family medicine specialist whose career has centered on the medical needs of unhoused people and jail inmates in the St. Louis area.
“What we’re trying for is to make it accessible over the counter much as we have Narcan accessible over the counter with the standing order,” Rottnek says. “What’s cool about this approach is this is one way people can stay alive and maybe one more avenue to get into treatment.”
Rottnek, a professor and the director of community medicine at Saint Louis University School of Medicine, points out that last year the Missouri General Assembly passed a law to allow anyone to get emergency HIV medication at a pharmacy without a prescription.
“So there is precedent in Missouri to allow that to happen,” Rottnek says, alluding to Rehder’s bill.
Meanwhile, the scope of America’s opioid crisis continues to worsen. In addition to the 100,000 Americans who died last year from drug overdoses, at least ten times that number are estimated to have survived non-fatal overdoses.
What’s more, at least 1 million Medicare beneficiaries suffer from an opioid use disorder, according to a December report issued by the Office of Inspector General for the U.S. Department of Health and Human Services.
Rottnek envisions family members getting involved in the event Rehder’s bill is passed into law and naltrexone is given out in pill form to people in recovery.
“You know the way that moms make sure their kids take their antibiotics — it’s to take it in front of them every day, right?” Rottnek says.
Making naltrexone available over the counter would only be a first step, Rottnek says.
“And then what the second step would be is really creating an educational campaign for the public to understand this prophylactic piece,” he says.
“It’s the same with Narcan,” Rottnek adds. “A lot of moms get Narcan through pharmacies.”

A dog tag Daniel Coverdell wears telling emergency responders he is on naltrexone, since the treatment drug makes him resistant to opioid pain relievers. // Photo by Theo Welding
Jenny Armbruster, deputy executive director of PreventEd, one of the St. Louis region’s leading sources of drug policy information, reserved judgment on Rehder’s bill.
“Will this be the answer?” Armbruster says. “No, nothing is the answer. But I think we have to explore a variety of strategies and figure out what’s going to work best for different people. And that’s going to be different answers.”
Ben Westhoff in 2019 published a book about how fentanyl had taken over America’s market for illegal drugs. (Editor’s note: After the reporting of this story, Westhoff was named executive editor of Euclid Media Group weeklies, which includes the Riverfront Times. He was not involved in the editing or writing of this story.)
Westhoff can vouch for the effectiveness of Vivitrol as a way to deter opioid dependence based on the experience of a friend released from prison last summer.
“Since he’s gotten out, he’s been on the Vivitrol shot,” says Westhoff, the author of Fentanyl, Inc: How Rogue Chemists Are Creating the Deadliest Wave of the Opioid Epidemic. “And it’s really helped him so far. Knock on wood. It’s a long-term process.”
Some addiction specialists hope that the opioid epidemic will follow the trajectory of tobacco use in America. Once cheap and ubiquitous, cigarettes and other tobacco products have fallen out of favor in most of the country, the result of school education programs, anti-smoking ordinances and high government taxes.
But Westhoff sees a problem with that analogy because “fentanyl is really a supply-driven problem rather than a buyer-driven problem,” he says. “A lot of people taking fentanyl and dying from it aren’t even aware that they’ve taken it.”
As for ending the record-setting number of drug overdose deaths in America, Westhoff sees little reason for optimism.
“I think the number of deaths is going to keep going up in the coming years,” he says. “Because previously fentanyl was adulterating heroin, and not all that many Americans use heroin. But now that it’s gotten into pills, it’s a much bigger market. Many more people use pills.”
He adds that education is the key.
“Any pill or powder bought on the black market could have fentanyl in it,” he says. “And I don’t think most people know that.”
Schwarz, the Wash U School of Medicine addiction specialist, sees reason to feel optimistic about progress in slowing the momentum of the drug overdose epidemic.
One sign is the fact that Rehder is even sponsoring a bill to widen access to naltrexone.
“I think it’s a step in the right direction,” Schwarz says. “Eight years ago, we wouldn’t have had this.”
Another hopeful sign is the fact, he says, that “more attention is being paid to substance use disorder and the stigma surrounding it, which makes me optimistic that eventually we can get to a better place than we have been in the past.”
Schwarz pauses to add a big caveat.
“It’s going to be, unfortunately, slow.”
This piece was republished with permission from our sister publication in St. Louis, Riverfront Times.